LEADER IN THE NEUROTECH SPOTLIGHT: FRANZ BOZSAK, CEO & CO-FOUNDER, SENSOME
ABOUT LIZ MOYLES – HEAD OF NEUROTECH, CRUXX, AUTHOR
Liz Moyles is a self-described frustrated neurosurgeon. A lengthy hospital stay in her teenage years left her with PTSD and a fear of hospitals and blood, rerouting her career path entirely at 18.
Medicine was the plan. Biochemistry became the reality. But life in a lab was not where she belonged. What never left her was her fascination with the brain and the people building in the space.
Today, as Head of Neurotech at Cruxx, she works with start-ups and scale-ups across the US, Europe and beyond to help them attract the talent and capital required to build.
Her aim is simple: to give CEOs and leadership teams their time back to operate at a strategic level, not get pulled into day-to-day execution.
Fundraising, clinical trials, and regulatory work already stretch teams thin. Hiring sits on top of all of it.
When it goes wrong or moves too slowly, the consequences are immediate. It can mean missing funding, delaying submissions, slipping milestones, or losing people through overload.
Liz leads global executive searches for VCs and neurotech companies, placing C-suite and board-level leaders and building out senior teams across the US, Europe and beyond.
Embedded in the neurotech ecosystem, she speaks regularly with founders, operators, KOLs and investors, giving her a clear view of where the field is heading and what it takes to succeed in a start-up. That perspective shapes how she approaches hiring.
In start-ups, every hire matters, and attracting the best is non-negotiable. But they are rarely looking. Busy building elsewhere and often unaware of what you’re doing.
Finding them is one challenge. Getting them to engage is another.
But while you and your hiring managers are trying to find these people, the clock is running. FDA submissions, fundraising rounds, clinical trials.
Everything that cannot wait is …………waiting.
Reach out to Liz. That person is out there. She knows the space and where to find the people.
They just don’t know you exist. Yet!

This week Sensome have announced another key milestone.
First-in-human stroke results have been published in the Journal of NeuroInterventional Surgery.
I am resharing my original interview with Franz Bozsak, CEO & Co-Founder of Sensome, as many of the milestones he promised us he would deliver in 2026 have come to pass.
When we spoke in December, Franz referred to them in the future tense.
Since then, we have heard.
January 2026: Sensome presented peripheral artery disease data at LINC 2026.
March 2026: Sensome and Robocath announced a robotic thrombectomy proof-of-concept integrating Clotild with Robocath’s R-ONE system.
May 2026: first-in-human stroke results published in the Journal of NeuroInterventional Surgery, showing that Sensome’s Clotild Smart Guidewire System can characterise clot from inside a fully occluded brain vessel during mechanical thrombectomy.
What makes the original interview more interesting now is not simply that milestones arrived. It is that many of the deeper themes Franz discussed are beginning to materialise publicly.
-The distinction between imaging and sensing.
-The idea that interventional medicine may eventually require real-time biological intelligence inside the body, not simply better external visualisation.
-The convergence of sensing, robotics, hardware, and AI inside procedural medicine.
Many may see the recent JNIS publication as a stroke-device milestone. But this is more.
Sensome are building a broader tissue-intelligence sensing platform spanning stroke, peripheral artery disease, and lung cancer intervention.
At present- outcome improvement has not yet been proven. The next critical step is demonstrating that real-time tissue sensing changes procedural decisions and improves patient outcomes during intervention.
That study still needs to happen.
But rereading this interview now, it is striking how many of the strategic milestones Franz described is beginning to emerge in real time.
Here is my original interview with Franz Bozsack. Well done Franz and looking forward to you completing all your milestones!
Minimally invasive intervention has transformed modern medicine. In stroke care, Mechanical Thrombectomy has shifted outcomes in ways that would have been unimaginable a generation ago.
Yet even in today’s advanced cath labs, physicians remain dependent on imaging that cannot fully reveal the biological nature of what they are treating.
Franz Bozsak, CEO and Co-Founder of Sensome, believes the next evolution of interventional medicine lies not in new mechanics, but in real-time biological intelligence.
By embedding microsensing technology directly into a neurovascular guidewire, Sensome aims to move physicians beyond silhouettes and toward tissue-level insight during the procedure itself.
I was fortunate enough to run into Franz in between the many conferences, clinical and regulatory commitments and his day job and I took the chance to bribe him with a coffee so I could do a deep -dive into him and Sensome.
In this conversation, Franz reflects on building what many initially thought was impossible, the transition from scientific validation to clinical impact, and why the future of MedTech will require hardware and AI to work as one.
Minimally invasive intervention has transformed modern medicine. In stroke care, Mechanical Thrombectomy has shifted outcomes in ways that would have been unimaginable a generation ago. Yet even in today’s advanced cath labs, physicians remain dependent on imaging that cannot fully reveal the biological nature of what they are treating.
Franz Bozsak, CEO and Co-Founder of Sensome, believes the next evolution of interventional medicine lies not in new mechanics, but in real-time biological intelligence. By embedding microsensing technology directly into a neurovascular guidewire, Sensome aims to move physicians beyond silhouettes and toward tissue-level insight during the procedure itself.
I was fortunate enough to run into Franz in between the many conferences, clinical and regulatory commitments and his day job and I took the chance to bribe him with a coffee so I could do a deep -dive into him and Sensome.
In this conversation, Franz reflects on building what many initially thought was impossible, the transition from scientific validation to clinical impact, and why the future of MedTech will require hardware and AI to work as one.

WHEN IMAGING ISN’T ENOUGH
Liz: Franz, can you start by explaining what Sensome does and the problem it was built to solve?
Franz: Minimally invasive treatments have revolutionized medicine over the past century, shifting us from open surgery to precise, less traumatic procedures. However, this revolution has made physicians heavily dependent on imaging, which often falls short of delivering the full picture.
In mechanical thrombectomy of acute ischemic stroke, for instance, angiography guides the physician to the blocked vessel effectively.
Yet contrast-enhanced fluoroscopic images reveal little about the occlusion, for example a clot’s exact in situ position, which is critical for maximizing recanalization success.
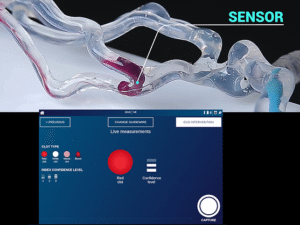
At Sensome, we have pioneered a microsensor technology that transcends imaging limits, delivering real-time biological intelligence.
Our breakthrough integrates the world’s smallest impedance-based sensor with proprietary predictive algorithms to characterize tissues in situ and in real time.
By embedding this ultra-miniaturized sensor into a workhorse neurovascular guidewire, we aim to empower neuro-interventionalists with precise occlusion details during the procedure.
This would enable optimal decision-making, enhancing patient outcomes right at the point of care.
It is like adding colour, texture, and dimensions to an image.
RETHINKING THE FIRST PASS
Liz: How does your solution compare to the current standard of care in mechanical thrombectomy?
Franz: Currently, mechanical thrombectomy involves navigating the treatment device, such as a stentriever or aspiration catheter, over a wire to the occluded vessel, guided by angiography.
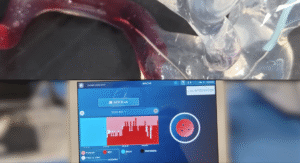
By integrating our sensor technology into a standard workhorse guidewire, we do not change the existing workflow while delivering critical in situ insights during navigation.
For instance, this approach could allow physicians to reveal the true location of the proximal interface of the clot, thereby facilitating the optimal placement of the aspiration catheter in direct contact with the clot.
This would, in turn, increase the likelihood of achieving a first-pass effect.
BUILDING THE “IMPOSSIBLE” SENSOR
Liz: Looking back, what achievement at Sensome are you most proud of, particularly in terms of impact on clinicians and patients?
Franz: When I founded Sensome, I was told that the sensor I envisioned was impossible to build.
Today this “impossible” sensor has safely been used in over 80 patients across 3 indications, namely endovascular treatment of acute ischemic stroke and peripheral vascular disease, as well transbronchial biopsy for lung cancer diagnosis.
Developing this miniaturized sensor was no small feat and integrating it with a high-performance neurovascular guidewire presented significant additional challenges.
Having succeeded to build an “impossible” technology that has the potential to serve millions of patients across multiple indications, is certainly our team’s proudest achievement.
THE PIVOT FROM PROOF TO IMPACT
Liz: What will be the markers of success for you and your team in 2026?
Franz: It is going to be a pivotal year for Sensome as we move from establishing the science of tissue sensing to demonstrating the impact that detailed information on clots and tissues can have on procedures and patients.
Over the past couple of years, we completed clinical studies across the three indications. In each domain, we demonstrated that our proprietary tissue sensing technology is capable of safely bringing valuable insights to these clinical procedures.
This year, we are ready to bring these results to the medical community.
We started the year with a presentation of our peripheral vascular results at the prestigious LINC 2026, a few months from now our lung cancer research will follow at ATS, and our ischemic stroke data will be published in early 2026.
With the scientific foundation set, we are ready to start showing how tissue sensing will transform these procedures: leading the way in evidence generation will be our program in the treatment of ischemic stroke.
The tissue and clinical data obtained from our technology will directly be feeding into what will eventually become an AI companion providing insights to support physicians during mechanical thrombectomy.
This has the potential to ensure the best results for their patients no matter if the patient is having a stroke in a metropolitan area or in the countryside.

THE NEXT FRONTIER: PHYSICAL AI
Liz: Looking more broadly at NeuroTech, what trends do you believe we will see over the next year?
Franz: Over the past few years, AI in Medtech mostly meant software-based AI based on text or imaging. We are now moving to the most exciting frontier: Physical AI.
The field where the “rubber hits the road” and AI must work in conjunction with hardware to treat patients.
At the interface of this marriage of hardware and software sits a sensing layer that translates the physical world for the AI, making the robot “feel”.
And Sensome is ready and excited to lead this next revolution by providing real-time in situ information during interventional procedures for the very first time.
The ARPA-H call for the development of Autonomous Interventions and Robotics is a clear sign that policymakers and healthcare officials have understood the importance and the need for this next step in MedTech.
IS CONFIDENCE RETURNING TO MEDTECH?
Liz: What do you think we will see in funding trends this year?
Franz: The year started with a bang thanks to the announcement of the Penumbra acquisition by Boston Scientific. Boston is continuing its buying spree of the past few years, adding a crown jewel of vascular intervention to its portfolio.
Might this be the sign we have been waiting for that indicates the turn-around when the markets start opening up again?
Several companies are looking to go public this year, and it seems the strategics are ready to make new bets again. All this would clearly bring back much needed confidence in MedTech investments.
STROKE IS ONLY THE BEGINNING
Liz: Which neurological conditions do you believe are closest to seeing real shifts in standard of care?
Franz: Over the past decade, acute ischemic stroke treatment has undergone a remarkable transformation: from a condition brutally constrained by time windows to one of medicine’s most effective interventions.
But AIS treatment only starts with reopening the artery and optimal long-term outcomes hinge on what follows: the rehabilitation phase.
Big corporations as well medical device entrepreneurs recognize this and are working on solutions that accompany the patient on the journey from the stroke itself all the way back to independent living.
COLLABORATION AS A COMPETITIVE ADVANTAGE
Liz: What do you think we could achieve in the NeuroTech & MedTech start-up world by working together?
Franz: Working “together” is the key word here. We are all connected by the same goal of improving patients’ lives. Medtech is already hard on its own; there is no need to make things even harder by walking these paths alone.
Creating spaces where we can share our experiences with others and pass on our knowledge from one generation of entrepreneurs to the next is the best way to increase the impact of our innovations beyond our own projects.
I have found the MedTech entrepreneur community to be an extremely supportive and sharing one.

WHERE THE NEURO COMMUNITY GATHERS
Liz: For those planning their calendars, what do you see as must-attend events in the neuro space?
Franz: BRAIN conference at the end of the year in London.
CLOSING THOUGHTS
If the first era of minimally invasive stroke care was defined by imaging, the next may be defined by biological intelligence.
Sensome’s work sits at a critical inflection point: moving from proving that tissue sensing is possible to demonstrating how it meaningfully changes procedural outcomes. As hardware, sensing, and AI begin to converge inside the interventional suite, the boundary between mechanical execution and data-driven decision-making will continue to narrow.
Whether 2026 becomes the year that tissue intelligence reshapes thrombectomy will depend on evidence, adoption, and continued collaboration across the MedTech ecosystem. But one thing is clear: the conversation is no longer just about accessing the vessel – it is about understanding what lies within it.
EDITORIAL NOTE | MAY 2026
Since this interview was first published, several of the milestones discussed above have materialised publicly.
Sensome presented peripheral artery disease data at LINC 2026, announced a robotic thrombectomy proof-of-concept with Robocath in March 2026, and published first-in-human stroke results in the Journal of NeuroInterventional Surgery in May 2026.
What is striking in retrospect is how much of the broader thesis discussed here is now beginning to emerge: the shift from external imaging toward real-time intraprocedural sensing, and the convergence of sensing, robotics, hardware, and AI inside intervention.
The key unanswered question remains the same: can tissue intelligence improve procedural outcomes in real-world thrombectomy?
That evidence still needs to be generated. But the conversation is no longer theoritical.



